Introduction
Every year, U.S. healthcare providers submit billions of medical claims — and a staggering portion of them are denied, delayed, or returned for corrections. The financial and operational consequences are enormous. Revenue leakage, administrative overload, and compliance risks are just a few of the pain points that emerge when claims management healthcare systems fail to perform at their best.
Whether you are a hospital administrator, a billing professional, a health plan executive, or a technology vendor, understanding how claims management works — and how to make it work better — is not optional. It is a strategic imperative.
This comprehensive guide walks you through every dimension of claims management in the healthcare industry. From the foundational claim cycle in medical billing to advanced claims management solutions, you will find actionable insights, practical frameworks, and expert guidance to help your organization reduce denials, accelerate reimbursement, and build a more resilient revenue cycle.
Let’s start from the beginning.
What Is Claims Management in Healthcare?
Claims management in healthcare refers to the end-to-end administrative and clinical process of submitting, tracking, adjudicating, and reconciling medical claims between healthcare providers and payers (insurance companies, government programs, or self-pay patients).
At its core, it answers one simple question: Did the provider get paid accurately and on time for the services they delivered?
But the process to answer that question is anything but simple. It involves:
- Patient registration and eligibility verification
- Accurate coding of diagnoses and procedures
- Clean claim submission to payers
- Real-time claim tracking and follow-up
- Denial management and appeals
- Payment posting and reconciliation
Claims management healthcare spans multiple departments — clinical, administrative, financial, and compliance — and touches every patient encounter from registration to final payment. When all of these moving parts align, the result is a healthy revenue cycle. When they don’t, organizations face claim rejections, revenue delays, and compliance exposure.
Medical Claims Management vs. General Claims Management
It is worth distinguishing medical claims management from general insurance claims management (e.g., auto or property insurance). While both involve submitting and processing claims, medical claims management operates within a uniquely complex regulatory and clinical environment.
Healthcare claims must comply with:
- HIPAA (Health Insurance Portability and Accountability Act) standards for electronic transactions
- ICD-10-CM/PCS and CPT coding systems
- CMS (Centers for Medicare & Medicaid Services) billing guidelines
- Payer-specific contract rules and coverage policies
This complexity is precisely why dedicated claims management solutions have become indispensable for healthcare organizations of all sizes.
Why Claims Management Healthcare Matters
The stakes in healthcare claims management are extraordinarily high — financially, operationally, and clinically.
The Financial Reality
According to industry reports, healthcare providers in the United States lose billions of dollars annually due to claim denials, inefficient billing processes, and write-offs. The American Medical Association (AMA) has consistently reported that claim denials cost physician practices and hospitals significant administrative resources to resolve.
Key financial impacts include:
- Revenue leakage: Claims that are denied and never resubmitted represent direct revenue loss.
- Cash flow disruption: Delayed payments strain operational budgets and capital planning.
- Administrative cost inflation: Manual follow-up on denied claims is labor-intensive and expensive.
- Write-offs: Claims that are too costly to appeal are written off, reducing net revenue.
Effective claims management healthcare practices directly counter each of these financial threats.
The Operational Reality
Beyond dollars and cents, poor claims management creates operational chaos:
- Billing staff spend excessive time on rework rather than clean claim submission.
- Providers face revenue uncertainty that complicates staffing, capital investment, and growth planning.
- Patient satisfaction suffers when billing errors lead to unexpected balances or delayed statements.
The Compliance Reality
Healthcare billing is one of the most heavily regulated areas of business. Errors in claims submission — intentional or accidental — can trigger audits, civil monetary penalties, or even exclusion from federal healthcare programs. A strong medical claims management framework is, therefore, also a compliance management strategy.
The Complete Claim Cycle in Medical Billing
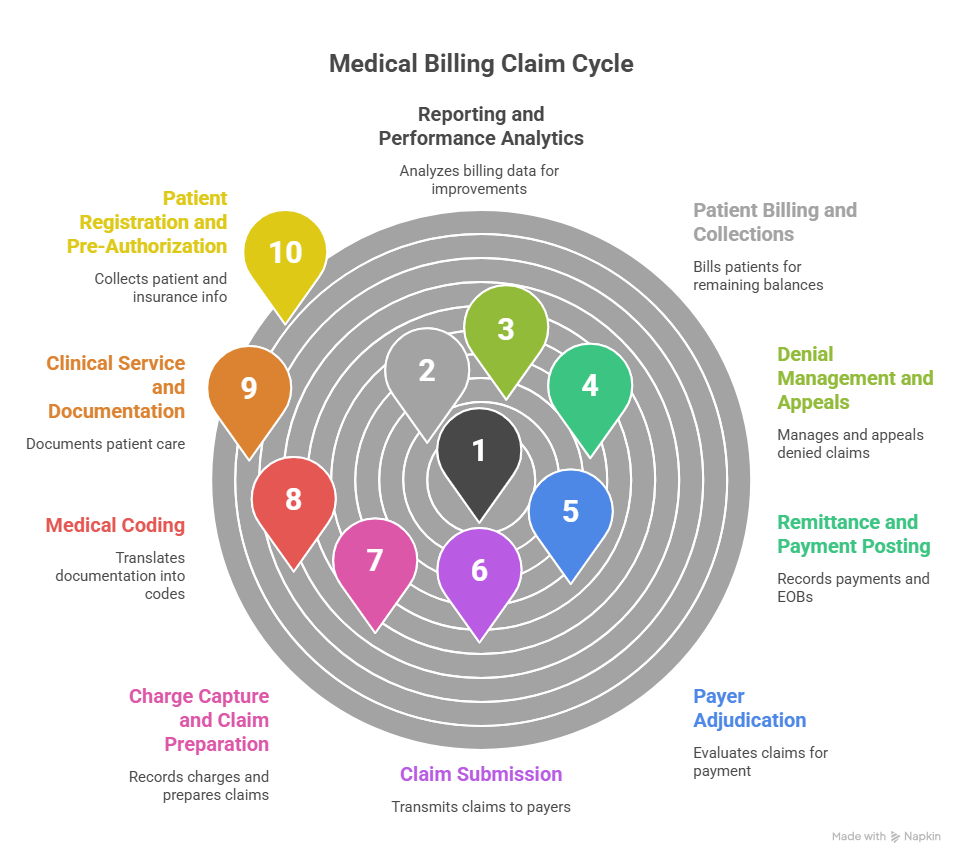
The claim cycle in medical billing describes the full journey of a healthcare claim — from the moment a patient schedules an appointment to the final resolution of their account. Understanding every stage of this cycle is essential for identifying where breakdowns occur and where improvements can be made.
Stage 1: Patient Registration and Pre-Authorization
The claim cycle begins before a single medical service is rendered.
Patient registration captures demographic and insurance information. Accuracy here is critical — errors in patient name, date of birth, insurance ID, or group number will cascade into claim rejections downstream.
Pre-authorization (or prior authorization) involves obtaining advance approval from the payer for specific services, procedures, or medications. Without it, certain claims will be automatically denied regardless of clinical necessity. This stage requires proactive communication between clinical staff, administrative teams, and the payer.
Best practices at this stage:
- Verify insurance eligibility in real time using automated eligibility verification tools.
- Confirm which services require prior authorization for each specific payer.
- Document all authorization numbers carefully and attach them to the claim.
Stage 2: Clinical Service and Documentation
Once the patient receives care, providers must document the encounter in a way that supports accurate billing. This is where clinical and administrative functions intersect.
Clinical documentation must capture:
- The patient’s chief complaint and presenting symptoms
- Relevant history, examination findings, and diagnostic results
- The clinical diagnosis (which maps to an ICD-10 code)
- The services, procedures, or treatments delivered (which map to CPT or HCPCS codes)
- Medical necessity justification
Thorough documentation is not just a billing requirement — it is a clinical and legal obligation. Gaps in documentation are one of the leading causes of claim denials.
Stage 3: Medical Coding
Medical coding translates clinical documentation into standardized codes that payers use to adjudicate claims. This is one of the most technically demanding stages of the claim cycle in medical billing.
Three primary code sets are used:
- ICD-10-CM/PCS — International Classification of Diseases codes that represent diagnoses (CM) and inpatient procedures (PCS).
- CPT (Current Procedural Terminology) — Codes maintained by the AMA that represent physician services and outpatient procedures.
- HCPCS Level II — Codes for supplies, equipment, drugs, and services not covered by CPT.
Common coding errors that derail the claim cycle:
- Upcoding or undercoding (billing for a higher or lower level of service than documented)
- Unbundling (billing separately for services that should be billed together)
- Incorrect modifier usage
- Diagnosis-procedure mismatch
- Missing specificity in diagnosis coding
Certified professional coders (CPCs) and certified coding specialists (CCSs) play a critical role in maintaining coding accuracy and compliance.
Stage 4: Charge Capture and Claim Preparation
Charge capture is the process of recording all billable services for a patient encounter and translating them into charges on the claim form. Incomplete charge capture — missing line items, incorrect units, or omitted services — leads to under-billing.
The claim is then prepared using standardized forms:
- CMS-1500: Used by physicians, outpatient facilities, and other non-institutional providers.
- UB-04 (CMS-1450): Used by hospitals and other institutional providers.
Electronic claims are transmitted in ANSI X12 EDI 837 format, with 837P for professional claims and 837I for institutional claims.
Stage 5: Claim Submission in Medical Billing
Claim submission in medical billing is the formal transmission of the completed claim to the payer for adjudication. This stage has evolved dramatically from paper-based processes to real-time electronic submission.
Claims can be submitted:
- Directly to the payer via the payer’s portal or EDI connection
- Through a clearinghouse, which acts as an intermediary that validates, routes, and reformats claims for different payers
Using a clearinghouse is the most common approach for practices billing multiple payers. Clearinghouses perform a first-pass edit check that catches formatting errors, missing data, and invalid codes before the claim reaches the payer — preventing rejections that would delay payment.
Stage 6: Payer Adjudication
Once the payer receives the claim, the adjudication process begins. The payer evaluates the claim against:
- The patient’s eligibility and coverage on the date of service
- The provider’s contract terms and fee schedule
- Medical policy and clinical coverage criteria
- Coordination of benefits rules (if the patient has multiple insurers)
- Utilization management requirements (e.g., prior authorization status)
The payer’s system applies automated edits and, for complex claims, routes the claim for manual review by a claims examiner. The outcome is one of the following:
- Approved/Paid: The claim is processed according to the contract rate.
- Partially approved: Some services are covered; others are denied.
- Denied: The entire claim or specific line items are rejected with a denial reason code.
- Suspended: The claim is held for additional review or information.
Stage 7: Remittance and Payment Posting
When the payer finalizes adjudication, it issues an Explanation of Benefits (EOB) to the patient and an Electronic Remittance Advice (ERA / 835 transaction) to the provider. The ERA details:
- What was billed
- What was allowed under the contract
- What the payer paid
- What was denied and why
- Patient responsibility amounts
Payment posting involves applying these remittance details to the patient account in the practice management system. Accurate and timely payment posting is essential for maintaining accurate AR (accounts receivable) balances and identifying underpayments.
Stage 8: Denial Management and Appeals
Denied claims do not have to be final. Denial management is the systematic process of:
- Identifying denied claims and their root causes
- Correcting errors (coding, documentation, eligibility)
- Submitting appeals or corrected claims within payer-specific timelines
- Tracking appeal outcomes and updating processes to prevent recurrence
This stage is where many organizations leave significant revenue on the table. Without a structured denial management workflow, denials pile up, appeal deadlines pass, and revenue is written off unnecessarily.
Stage 9: Patient Billing and Collections
After insurance adjudication, any remaining patient responsibility (deductibles, copays, coinsurance) is billed to the patient. Effective medical claims management includes a patient-friendly billing process that:
- Sends clear, itemized statements
- Offers multiple payment options (online portal, payment plans, phone)
- Complies with the No Surprises Act and other transparency regulations
- Escalates to collections only as a last resort
Stage 10: Reporting and Performance Analytics
The final stage of the claim cycle is analysis. Healthcare organizations that rigorously track key billing performance metrics can identify systemic issues, measure improvement over time, and optimize their revenue cycle proactively.
Claim Submission in Medical Billing: A Step-by-Step Breakdown
Claim submission in medical billing deserves deeper exploration because it is the pivotal action that initiates the payer’s adjudication process. Getting submission right — clean, complete, and timely — is the single most impactful way to accelerate reimbursement.
Step 1: Pre-Submission Validation (Claim Scrubbing)
Before a claim leaves the provider’s system, it should pass through a claim scrubber — a software tool that checks for:
- Missing or invalid patient demographics
- Invalid or expired insurance IDs
- Mismatched diagnosis and procedure codes
- Missing modifiers
- Invalid place-of-service codes
- Duplicate claims
- Fee schedule and bundling rule violations
Claim scrubbing is the first line of defense against rejections. Modern claims management solutions include sophisticated scrubbing engines that apply thousands of payer-specific edits in real time.
Step 2: Clearinghouse Submission and Acknowledgment
After scrubbing, the claim is transmitted to a clearinghouse. The clearinghouse:
- Validates the claim’s format and data elements
- Routes it to the appropriate payer
- Returns a 999 acknowledgment transaction confirming receipt
- Returns a 277CA (Claim Acknowledgment) transaction indicating whether the payer accepted or rejected the claim
Any claims flagged as rejected at this stage must be corrected and resubmitted — they never entered the payer’s system, so the adjudication clock has not started.
Step 3: Payer Acceptance and Tracking
Once the payer accepts the claim, providers can track its status using the 276/277 transaction set (Claim Status Request/Response). Modern clearinghouses and practice management systems automate this status tracking, alerting billing staff when claims are held, additional information is requested, or adjudication is complete.
Step 4: Timely Filing Compliance
Every payer has a timely filing deadline — the window within which claims must be submitted after the date of service. Missing these deadlines results in a timely filing denial, which is almost always non-appealable.
Common timely filing limits:
- Medicare: 12 months from the date of service
- Medicaid: Varies by state (often 90–365 days)
- Commercial insurers: Typically 90–180 days, but varies by contract
A robust claims management system tracks timely filing deadlines and flags at-risk claims proactively.
Step 5: Secondary and Tertiary Claim Submission
When a patient has more than one insurance plan, coordination of benefits (COB) rules determine which payer is primary and which is secondary. After the primary payer adjudicates the claim, the EOB or ERA is used as a crossover document to bill the secondary payer for the remaining balance.
This multi-payer billing process adds complexity but can significantly reduce the patient’s out-of-pocket responsibility — and maximize provider reimbursement.
Healthcare Claims Processing: From Submission to Payment
Healthcare claims processing is the payer-side counterpart to provider claims management. Understanding how payers process claims helps providers anticipate adjudication decisions and minimize denials.
How Payers Process Claims
When a payer receives a claim, it passes through multiple processing queues:
Auto-adjudication handles the majority of straightforward claims through automated rules engines. Claims that meet all criteria are approved and paid without human review — often within 14–30 days of submission.
Pended claims are routed for additional review when they trigger specific edit rules, require medical necessity review, or involve complex benefits. Pended claims may require:
- Submission of medical records
- Certificate of Medical Necessity
- Operative reports or pathology results
- Coordination of benefits documentation
Denied claims are returned with an Explanation of Benefits and standardized CARC (Claim Adjustment Reason Codes) and RARC (Remittance Advice Remark Codes) that explain the denial reason.
Key Payer Adjudication Rules
Understanding payer adjudication rules helps providers submit cleaner claims:
- National Correct Coding Initiative (NCCI) edits: CMS-developed code pair edits that prevent unbundling of services.
- Medically Unlikely Edits (MUEs): Limits on the units of service that can be billed per day per code.
- Local Coverage Determinations (LCDs) and National Coverage Determinations (NCDs): Payer-specific and CMS-mandated rules on covered diagnoses for specific services.
- Global surgery rules: Prohibit separate billing for pre- and post-operative care within a defined global period.
Electronic Data Interchange (EDI) in Healthcare Claims Processing
EDI is the electronic exchange of standardized business documents between healthcare entities. HIPAA mandates the use of specific EDI transactions for claims management:
| Transaction | Purpose |
| 837P / 837I | Electronic claim submission (professional / institutional) |
| 835 | Electronic Remittance Advice (payment explanation) |
| 270/271 | Eligibility inquiry and response |
| 276/277 | Claim status request and response |
| 278 | Prior authorization request |
| 999 | Acknowledgment (claim received) |
| 277CA | Claim acknowledgment (accepted/rejected) |
Mastery of these EDI transactions is foundational to efficient healthcare claims processing.
Common Challenges in Medical Claims Management
Even well-resourced healthcare organizations struggle with persistent challenges in medical claims management. Identifying these challenges is the first step to overcoming them.
1. High Claim Denial Rates
Denial rates in healthcare typically range from 5% to 15%, with some specialties and settings experiencing even higher rates. Common denial reasons include:
- Eligibility denials: Coverage not active on the date of service
- Authorization denials: Required prior authorization not obtained
- Coding denials: Invalid, unsupported, or bundled codes
- Duplicate claim denials: Claim submitted more than once
- Timely filing denials: Claim submitted past the deadline
- Medical necessity denials: Service not covered for the stated diagnosis
Each denial type requires a different root-cause analysis and corrective action strategy.
2. Staffing Shortages and High Turnover
Medical billing is a specialized skill. Shortages of experienced coders and billing staff create workflow bottlenecks, increase error rates, and slow down denial follow-up. High turnover compounds the problem by requiring constant recruiting, hiring, and training investment.
3. Payer Complexity
Managing billing relationships with dozens of payers — each with unique coverage policies, fee schedules, authorization requirements, and claim formats — is operationally demanding. Payer rule changes occur frequently, and failure to stay current results in avoidable denials.
4. Coding Complexity and Compliance Risk
The ICD-10-CM code set alone contains over 70,000 codes. Coding accurately and specifically requires clinical knowledge, ongoing education, and meticulous documentation. Coding errors — especially upcoding — create compliance risk under the False Claims Act.
5. Technology Fragmentation
Many healthcare organizations operate multiple disconnected systems: an EHR, a practice management system, a billing system, and a clearinghouse portal. Data silos between these systems create manual reconciliation work, data entry errors, and visibility gaps.
6. Underpayment Detection
Payers do not always reimburse providers at contracted rates. Systematic underpayments — paying less than what the contract stipulates — can go undetected without robust payment posting and contract management tools. Industry estimates suggest that a meaningful percentage of provider payments are underpaid.
7. Regulatory Change Management
Healthcare billing regulations evolve constantly: annual ICD-10 updates, CPT code changes, CMS policy revisions, state Medicaid rule changes, and new federal legislation (e.g., the No Surprises Act, price transparency rules). Keeping up requires dedicated compliance monitoring resources.
Top Claims Management Solutions for Healthcare Organizations
The right claims management solutions can transform a struggling revenue cycle into a high-performing one. Solutions range from standalone billing tools to comprehensive revenue cycle management (RCM) platforms.
1. Clearinghouse Services
A healthcare clearinghouse is the backbone of electronic claim submission in medical billing. Top clearinghouses include:
- Change Healthcare (Optum): One of the largest clearinghouses in the U.S., offering extensive payer connectivity, claim scrubbing, and analytics.
- Availity: Widely used for real-time eligibility verification and claim status tracking.
- Waystar: Known for strong denial management and analytics capabilities.
- Trizetto (Cognizant): Offers clearinghouse services integrated with payer and provider solutions.
What to look for in a clearinghouse:
- Payer network breadth (how many payers they connect to)
- Real-time claim status tracking
- Claim editing and scrubbing capabilities
- EDI support and companion guides
- Rejection and denial reporting
2. Practice Management Systems (PMS)
A Practice Management System is the administrative hub for scheduling, billing, and reporting. Many PMS platforms include integrated claims management functionality:
- Epic Resolute: Comprehensive billing module used by large health systems.
- Athenahealth: Cloud-based platform with strong clearinghouse integration and denial management.
- AdvancedMD: Popular with mid-size and specialty practices.
- Kareo / Tebra: Designed for small practices and independent providers.
3. Revenue Cycle Management (RCM) Software
Comprehensive RCM platforms manage the entire claim lifecycle from eligibility verification to final payment. They typically include:
- Patient access and registration tools
- Real-time eligibility verification
- Coding assistance and charge capture
- Claim scrubbing and submission
- Denial management workflows
- Payment posting and reconciliation
- Analytics and reporting dashboards
Leading RCM platforms include Meditech, Cerner Revenue Cycle, nThrive, Parallon, and R1 RCM.
4. AI-Powered Coding Assistance
Artificial intelligence tools are transforming medical coding by:
- Analyzing clinical documentation and suggesting appropriate codes
- Flagging coding opportunities that human coders may miss
- Identifying compliance risks and documentation gaps
- Automating routine coding tasks to improve coder productivity
Companies like Nuance (Microsoft), Optum360, and 3M Health Information Systems offer AI-assisted coding solutions that integrate with EHR platforms.
5. Denial Management and Appeals Tools
Specialized denial management platforms help organizations:
- Categorize and prioritize denials by payer, denial reason, and dollar value
- Automate appeal letter generation
- Track appeal status and outcomes
- Identify denial trends and root causes
- Measure denial rate reduction over time
6. Outsourced Medical Billing Services
Many healthcare organizations — particularly smaller practices — choose to outsource their billing and medical claims management to third-party revenue cycle management companies. Outsourcing can:
- Reduce administrative overhead and staffing costs
- Provide access to specialized coding and billing expertise
- Improve denial management capabilities
- Offer scalability without fixed headcount
When evaluating outsourced RCM vendors, assess their experience with your specialty, technology infrastructure, denial management performance, and transparent reporting.
Technology Driving Modern Claims Management
The claims management healthcare landscape is being fundamentally reshaped by technology. Organizations that embrace these innovations gain a significant competitive advantage.
Artificial Intelligence and Machine Learning
AI and ML are being applied across the claims management lifecycle:
- Predictive denial management: AI algorithms analyze historical denial data to predict which claims are likely to be denied before submission, allowing for proactive correction.
- Automated coding: Natural language processing (NLP) models extract clinical concepts from physician notes and map them to appropriate codes.
- Fraud detection: ML models identify unusual billing patterns that may indicate fraud, waste, or abuse.
- Prior authorization automation: AI tools predict authorization requirements and automate the submission of prior authorization requests.
Robotic Process Automation (RPA)
RPA uses software bots to automate repetitive, rule-based tasks that previously required human intervention:
- Eligibility verification across multiple payer portals
- Claim status checking and follow-up
- Payment posting from ERAs
- Generating and sending appeal letters
- Reconciling payer remittances with expected payments
RPA reduces manual effort, minimizes errors, and allows billing staff to focus on higher-value activities like complex denial management and patient communication.
Cloud-Based RCM Platforms
Cloud-based claims management solutions offer advantages over legacy on-premise systems:
- Real-time data access from any location (critical for remote billing teams)
- Automatic software updates (ensuring payer rule changes are reflected promptly)
- Scalability to handle volume fluctuations
- Lower upfront capital costs
- Enhanced data security and disaster recovery
Interoperability and FHIR Integration
The HL7 FHIR (Fast Healthcare Interoperability Resources) standard is enabling seamless data exchange between EHRs, practice management systems, clearinghouses, and payers. Improved interoperability means:
- Clinical data flows directly to the billing system without manual re-entry
- Real-time eligibility and authorization data is embedded in the clinical workflow
- Payer adjudication results are automatically posted to the patient account
CMS’s interoperability rules are driving broader adoption of FHIR-based APIs across the industry.
Telehealth Billing Integration
The explosive growth of telehealth services has introduced new billing complexities — new CPT codes, modifier requirements, place-of-service variations, and payer-specific telehealth coverage policies. Modern claims management solutions now include telehealth billing modules that handle these unique requirements.
Best Practices for Optimizing Claims Management
Regardless of the size or type of your healthcare organization, these best practices will strengthen your claims management healthcare performance.
1. Invest in Front-End Revenue Cycle Processes
The most effective way to prevent claims problems is to address them before the claim is ever submitted. Focus on:
- Real-time eligibility verification at every patient access touchpoint (scheduling, pre-registration, day of service)
- Proactive prior authorization management with clear workflows and responsibility assignments
- Accurate patient demographic collection with address verification and ID scanning tools
- Financial counseling to inform patients of their expected out-of-pocket responsibility before service
Studies consistently show that every dollar invested in front-end revenue cycle processes saves multiples in downstream denial management and rework costs.
2. Establish a Claims Denial Tracking System
You cannot manage what you do not measure. Build a denial tracking system that captures:
- Denial date, payer, and denial reason code
- Original claim date and amount
- Action taken and outcome
- Days to resolution
- Revenue recovered vs. written off
Use this data to calculate your denial rate by payer, denial reason, and provider — and set targets for continuous improvement.
3. Create Payer-Specific Billing Guides
Each major payer in your portfolio has unique billing rules, coverage policies, and claim format preferences. Create internal billing guides for your top payers that document:
- Timely filing deadlines
- Prior authorization requirements
- Preferred claim formats and modifiers
- Contact information for provider relations and appeals
- Common denial reasons and resolution strategies
Update these guides whenever you receive payer communications about policy changes.
4. Implement a Denial Prevention Workflow
Rather than treating denial management as a purely reactive function, build proactive denial prevention into your daily workflow:
- Review your clearinghouse’s daily rejection and denial reports every morning
- Work denials within 24–48 hours to maximize appeal success rates
- Escalate high-value denials to senior billing staff or supervisors immediately
- Conduct weekly denial rounds to review trends and assign root-cause analysis tasks
5. Conduct Regular Coding Audits
Schedule internal coding audits — or engage external coding audit services — at least quarterly. Audits should:
- Sample claims across all major payers and providers
- Evaluate coding accuracy, documentation support, and compliance
- Identify training opportunities for coders and clinical staff
- Document findings and corrective action plans
Coding audits not only reduce denial risk but also protect against fraud and abuse investigations.
6. Train Clinical Staff on Documentation Standards
Physicians, nurses, and other clinical staff are not billers — but their documentation directly determines billing accuracy. Invest in:
- Regular clinical documentation improvement (CDI) training
- Provider-specific feedback reports on documentation deficiencies
- EHR templates that prompt for billing-relevant documentation elements
- Collaborative CDI specialist programs that work directly with clinical teams
7. Monitor and Manage Accounts Receivable Aging
Your AR aging report is one of the most important financial dashboards in your organization. Key benchmarks:
- Days in AR: Aim for under 40 days for most specialties
- AR over 90 days: Should represent less than 15–20% of total AR
- Denial rate: Target under 5% for high-performing organizations
- Net Collection Rate: Should approach 95–98% of contractually allowed amounts
Review AR aging weekly and assign ownership of buckets over 60 days to specific team members.
8. Leverage Technology Strategically
Do not implement technology for its own sake. Evaluate new tools against specific performance gaps:
- High denial rates → invest in AI-powered denial prediction and automated appeals
- Slow payment posting → implement ERA automation and RPA bots
- Coding errors → consider AI-assisted coding or CDI software
- Staff capacity constraints → evaluate outsourced RCM or offshore billing support
How to Choose the Right Claims Management Solution
With dozens of claims management solutions on the market, selecting the right one requires a structured evaluation process.
Step 1: Define Your Requirements
Start with a needs assessment:
- What is your current denial rate, and what are the primary denial reasons?
- How many claims do you submit per month, and to how many payers?
- What are your current technology systems (EHR, PMS), and what integration capabilities do they support?
- What is your budget for technology and/or outsourced services?
- Do you have in-house billing staff, or do you need a full-service solution?
Step 2: Evaluate Vendors Against Key Criteria
Build a vendor scorecard with these criteria:
- Payer connectivity: Does the solution connect to all your payers?
- EHR/PMS integration: Does it integrate natively or via API with your existing systems?
- Claim scrubbing quality: How many edits does the scrubbing engine apply? How current are they?
- Denial management capabilities: Does it provide root-cause analytics and workflow automation?
- Reporting and analytics: Can it deliver the KPIs you need to manage performance?
- Compliance updates: How quickly does the vendor update for regulatory and code changes?
- Customer support: What is the support model — dedicated account management, help desk, or self-service?
- References: Can the vendor provide references from organizations similar to yours?
Step 3: Request a Demonstration and Pilot
Do not make a purchase decision based on sales presentations alone. Request:
- A live demonstration using your actual claim types and denial scenarios
- A pilot or proof-of-concept with real data where possible
- Performance benchmarks and implementation timelines in writing
Step 4: Evaluate Total Cost of Ownership
Understand all costs involved:
- Implementation and configuration fees
- Monthly or annual subscription costs
- Per-claim transaction fees
- Training and onboarding costs
- Ongoing support and maintenance fees
Compare total cost of ownership (TCO) against the expected revenue impact — improved collection rates, reduced denial costs, and staff efficiency gains.
Key Metrics to Track in Healthcare Claims Processing
Measuring performance is essential in healthcare claims processing. These are the metrics every billing leader should monitor.
Financial Metrics
| Metric | Definition | Target |
| Days in AR (DAR) | Average time to collect from service date | < 40 days |
| Net Collection Rate | % of allowable revenue actually collected | ≥ 95% |
| Gross Collection Rate | Collections as % of gross charges | Varies by specialty |
| First-Pass Resolution Rate | % of claims paid on first submission | ≥ 90–95% |
| Denial Rate | % of claims denied by payers | < 5% |
| Denial Recovery Rate | % of denied claims successfully appealed | > 50% |
Operational Metrics
| Metric | Definition | Target |
| Claims Lag | Days from service to claim submission | < 3–5 days |
| AR Over 90 Days | % of total AR aged over 90 days | < 15% |
| Claim Rejection Rate | % of claims rejected by clearinghouse/payer | < 2% |
| Time to First Payment | Days from submission to first payment | < 30 days |
| Coder Accuracy Rate | % of claims coded without error | ≥ 95% |
Track these metrics monthly, trend them over time, and benchmark against industry standards for your specialty and organization type.
The Future of Claims Management in Healthcare
Claims management healthcare is evolving rapidly. Several trends will define the next decade.
Prior Authorization Reform
Prior authorization has long been one of the most burdensome aspects of healthcare billing. Legislative and regulatory pressure is mounting for payers to streamline and automate the prior authorization process. CMS has finalized rules requiring Medicare Advantage plans and Medicaid programs to implement electronic prior authorization using FHIR-based APIs — a major step toward reducing administrative burden.
Real-Time Claims Adjudication
Some payers are piloting real-time claims adjudication, where claims are submitted and adjudicated in near real-time during the patient encounter. This eliminates the multi-week wait that currently characterizes most claims processing and allows providers to collect patient balances at the point of care.
Value-Based Care and Alternative Payment Models
The shift from fee-for-service to value-based care is gradually changing the nature of claims management. Under bundled payments, capitation, or shared savings arrangements, providers are paid based on outcomes and population health metrics rather than individual services. This requires new billing and reporting capabilities — tracking quality metrics, reconciling shared savings, and managing risk-based contracts.
Expanded Use of AI and Automation
AI-driven automation will continue to expand across the claims management lifecycle — from AI-powered eligibility verification and prior authorization to automated claim resubmission and intelligent appeal management. Organizations that invest in AI-driven RCM tools now will be best positioned for the increasingly automated billing environment of the future.
Standardization and Interoperability
Ongoing federal interoperability initiatives — including CMS’s FHIR-based API rules and the Trusted Exchange Framework and Common Agreement (TEFCA) — will continue to drive standardization in data exchange. Greater standardization will reduce the administrative variation that currently makes multi-payer billing so complex.
Patient Financial Experience
As patient cost-sharing continues to rise, billing organizations will place greater emphasis on the patient financial experience — transparent cost estimates, digital payment tools, flexible payment plans, and proactive financial counseling. Patient-centric billing practices not only improve collections but also enhance patient satisfaction and loyalty.
FAQs: Claims Management in Healthcare
What is the difference between a claim rejection and a claim denial?
A claim rejection occurs before adjudication — the claim fails format or data validation checks and is returned to the provider without being processed. A claim denial occurs after adjudication — the payer received and reviewed the claim but determined it should not be paid. Rejections are corrected and resubmitted; denials may require appeals or corrected claims.
What is the claim cycle in medical billing?
The claim cycle in medical billing refers to the complete process from patient registration through final payment and account closure. It includes registration, pre-authorization, clinical documentation, coding, charge capture, claim submission, payer adjudication, remittance, denial management, patient billing, and reporting.
How long does healthcare claims processing take?
Most electronic claims are adjudicated within 14–30 days by commercial payers. Medicare typically adjudicates clean electronic claims within 14 days. Complex claims, pended claims, or claims requiring medical records may take 30–90 days or longer. Appeals can add additional weeks or months to the resolution timeline.
What is claim submission in medical billing?
Claim submission in medical billing is the formal process of transmitting a completed claim to the payer for adjudication. Claims are typically submitted electronically via a clearinghouse using the ANSI X12 837 transaction format. Clean claim submission — accurate, complete, and timely — is the key driver of fast reimbursement.
What are the most common reasons for medical claim denials?
The most common reasons include: patient eligibility issues, missing or invalid prior authorization, coding errors, timely filing violations, medical necessity denials, duplicate claims, and coordination of benefits issues. Addressing front-end revenue cycle processes reduces the majority of these denial categories.
What is a clearinghouse in medical billing?
A healthcare clearinghouse is an intermediary that receives electronic claims from providers, validates and reformats them, and routes them to the appropriate payer. Clearinghouses perform claim scrubbing, reduce rejections, and provide claim status tracking capabilities. They are a critical component of efficient claims management solutions.
How can I reduce my claim denial rate?
Key strategies include: verifying eligibility before every patient encounter, obtaining prior authorizations proactively, investing in coder training and quality audits, using claim scrubbing software, tracking denials by root cause, and building a structured denial management workflow with accountability metrics.
What is the No Surprises Act and how does it affect claims management?
The No Surprises Act (effective January 2022) protects patients from unexpected out-of-network medical bills in emergency situations and for certain non-emergency services at in-network facilities. It requires providers to give good faith cost estimates and establishes an independent dispute resolution process for payer-provider payment disagreements. Compliance with the Act requires updates to billing workflows, patient notification processes, and claim submission practices.
Conclusion
Effective claims management healthcare is one of the most powerful levers an organization can pull to improve financial health, reduce administrative waste, and ensure compliance. From mastering the claim cycle in medical billing to selecting the right claims management solutions, every step in the process represents an opportunity to optimize performance.
The organizations winning in today’s complex reimbursement environment are those that approach claims management strategically — investing in technology, training clinical and administrative staff, proactively preventing denials, and continuously measuring performance against industry benchmarks.
Whether you are rethinking your healthcare claims processing workflows, evaluating new technology platforms, or building out your denial management program, the principles in this guide provide a roadmap for sustainable improvement.
The claims management landscape will continue to evolve — driven by AI, interoperability mandates, value-based care, and rising patient financial responsibility. Organizations that build flexible, technology-forward, and data-driven billing operations today will be prepared to thrive in whatever environment comes next.Start with an honest assessment of where your current medical claims management process falls short. Then prioritize the highest-impact improvements. Even incremental gains in first-pass resolution rates, denial recovery, and AR days translate directly into stronger revenue and a more sustainable healthcare organization.
