Healthcare Accounts Receivable Process Guide
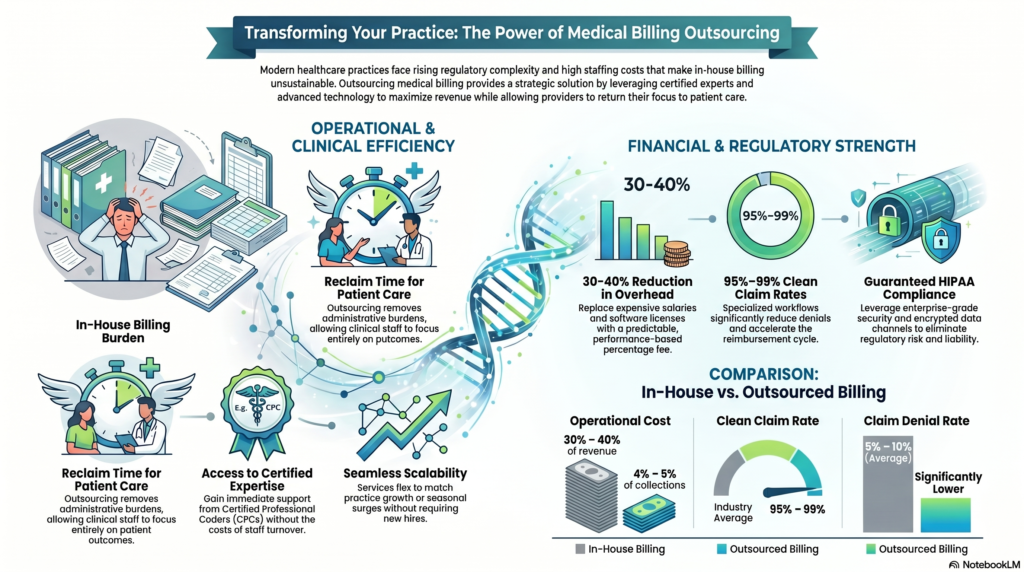
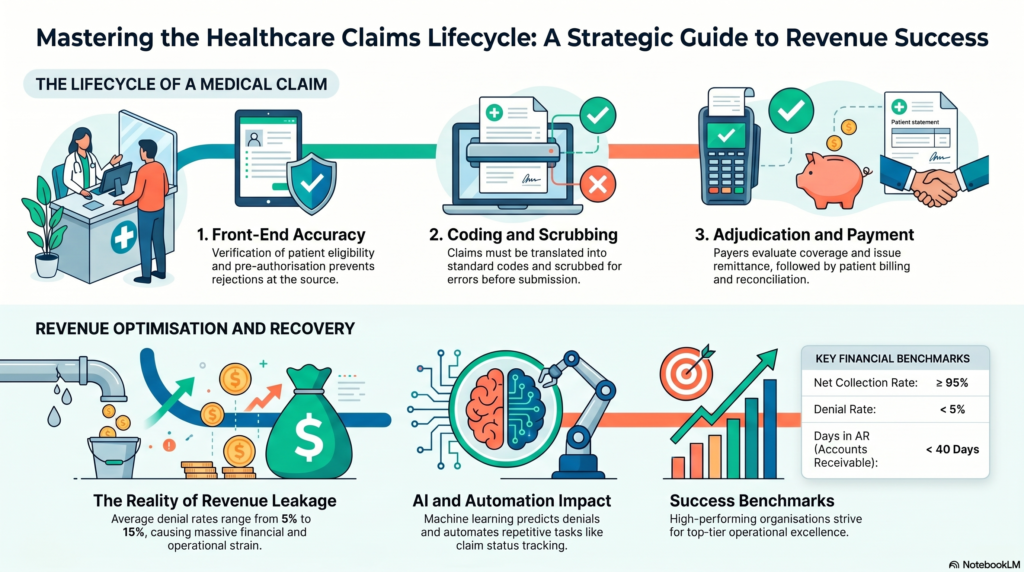
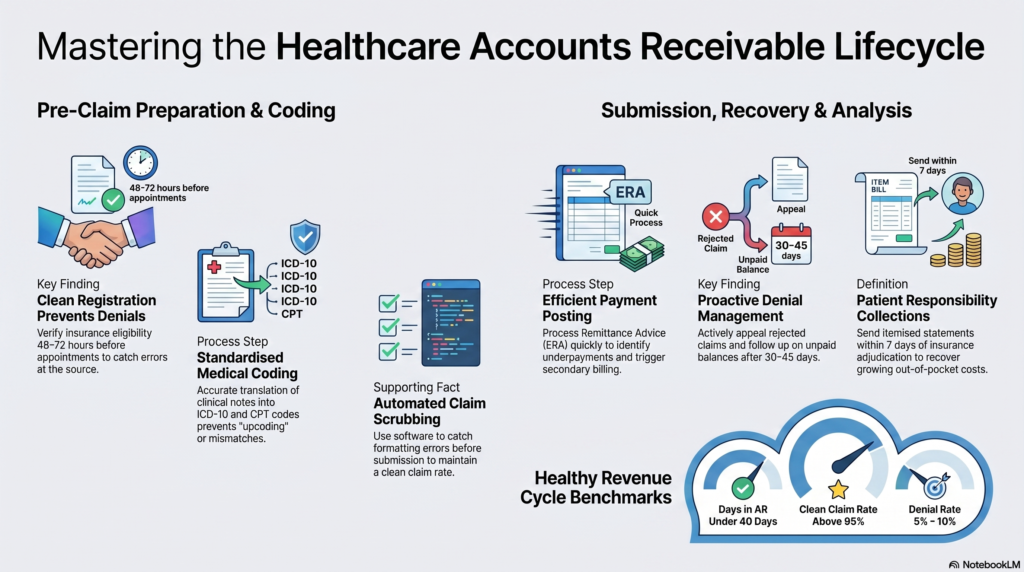
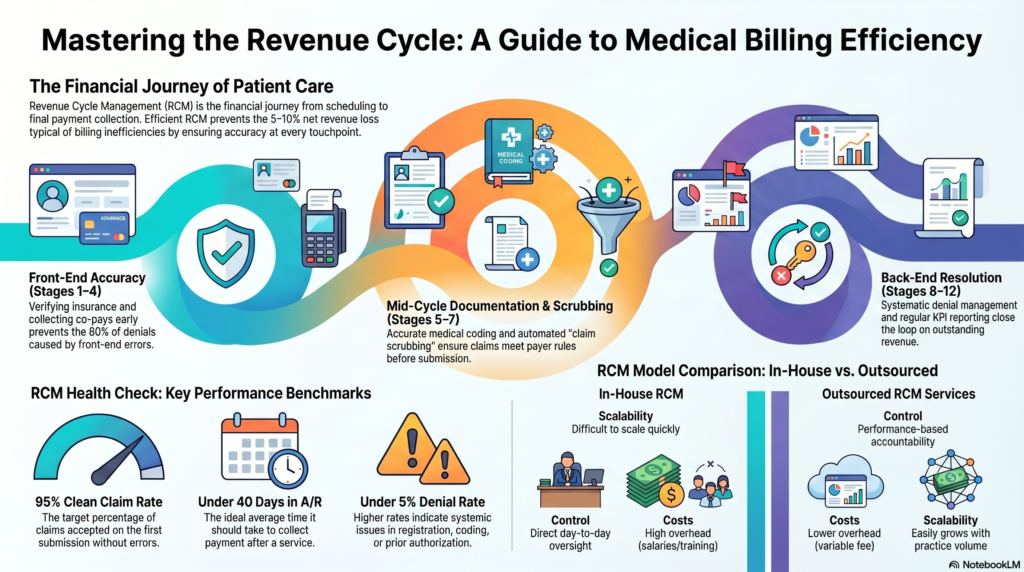
Introduction Every dollar a healthcare provider earns starts as a claim — and far too many of those claims never get paid on time. In fact, the American Medical Association reports that nearly 1 in 5 claims is initially denied or delayed, costing practices millions in lost or deferred revenue each year. That’s where healthcare accounts receivable management becomes mission-critical. Whether you run a small independent clinic or a large hospital system, understanding the full accounts receivable process in healthcare is the difference between a practice that thrives and one that constantly struggles with cash flow gaps. This guide breaks down everything — from the step-by-step AR workflow to the best medical accounts receivable solutions available today. You’ll walk away knowing exactly how to tighten your revenue cycle, reduce claim denials, and get paid faster for every service you deliver. What Is Healthcare Accounts Receivable? Healthcare accounts receivable refers to the money owed to a healthcare provider for services that have already been delivered but not yet paid. When a physician sees a patient, submits a claim, and waits for reimbursement from an insurance company or patient, that outstanding balance lives in the AR ledger until it’s collected. Think of AR as a running tab of earned revenue that hasn’t landed in your bank account yet. In most healthcare practices, AR balances come from three primary sources: Managing these balances efficiently is the core goal of healthcare accounts receivable management. A well-run AR process keeps aging balances low, denial rates minimal, and collection timelines as short as possible. Without a structured AR process, even high-volume practices can find themselves in a cash flow crisis — delivering care but waiting months (or never) to be reimbursed. The Accounts Receivable Process in Healthcare — Step by Step The accounts receivable process in healthcare is not a single event. It’s a multi-stage workflow that begins before the patient ever walks through the door and continues until every dollar owed is collected or written off. Here’s how it works: Step 1: Patient Registration and Insurance Verification Accurate AR management starts at the front desk. Collecting correct demographic information — name, date of birth, insurance ID, and group number — prevents costly errors downstream. Before the appointment, staff should verify: Failing to verify eligibility is one of the most common reasons claims get denied. This single step, when done correctly, eliminates a large percentage of preventable rejections. Step 2: Charge Capture After the patient is seen, the clinical encounter must be translated into billable charges. Physicians and clinical staff document services using: Accurate charge capture is essential. Under-coding leaves money on the table. Over-coding triggers audits and penalties. Clean, precise coding is the foundation of a strong accounts receivable medical billing workflow. Step 3: Claims Submission Once charges are captured and reviewed, the billing team submits claims to the appropriate payers. Most practices use electronic claim submission through clearinghouses, which scrub claims for errors before they reach the insurer. Claims are submitted on: Timely filing is critical. Most payers have strict deadlines — often 90 days to 1 year from the date of service. Missing those windows means automatic denial with no appeal option. Step 4: Payment Posting When payments arrive from payers or patients, they must be accurately posted to the correct patient accounts. Payment posting includes: Precise payment posting keeps your AR ledger accurate and ensures that patient statements reflect the correct balance owed. Step 5: AR Follow-Up and Denial Management This is where the real work of account receivable process in medical billing happens. Any claim not paid within 30–45 days needs proactive follow-up. The AR follow-up team should: We’ll cover denial management in more detail in a later section. Step 6: Patient Collections After insurance has paid its portion, any remaining balance is billed to the patient. The collections process includes: With patient financial responsibility rising due to high-deductible health plans, this step is increasingly important to overall collection rates. Step 7: Reporting and Analysis The final step is measuring everything. Regular AR reporting reveals: These insights fuel continuous improvement across the entire AR cycle. Key Metrics That Drive Healthcare AR Performance To manage what you can’t measure, you need to track the right KPIs. Strong healthcare accounts receivable management relies on these core metrics: Days in Accounts Receivable (DAR) This measures the average number of days it takes to collect payment after a service is provided. The industry benchmark is under 40 days. Anything above 50 days indicates systemic billing problems. Formula: Total AR ÷ (Annual Charges ÷ 365) First-Pass Claim Acceptance Rate This is the percentage of claims accepted and paid on the first submission — without correction or resubmission. A healthy rate is 95% or higher. Low first-pass rates signal coding errors, eligibility failures, or missing documentation. Net Collection Rate This measures the percentage of collectible revenue actually collected. It removes contractual write-offs from the equation and focuses on avoidable losses. Formula: (Payments ÷ (Charges − Contractual Adjustments)) × 100 A net collection rate below 95% means money is leaking out of your practice through denials, write-offs, and uncollected balances. Denial Rate The percentage of submitted claims denied by payers. Industry benchmark is under 5%. High denial rates directly reduce cash flow and inflate AR aging balances. Aging AR Percentage Track what percentage of your AR sits in each aging bucket. Ideally: When balances pile up in the 90+ day bucket, collectability drops sharply — many insurers and patients become nearly impossible to collect from after 120 days. Healthcare Accounts Receivable Management Best Practices Effective healthcare accounts receivable management isn’t about working harder — it’s about building smarter processes. These best practices separate high-performing revenue cycles from struggling ones: Prioritize Front-End Accuracy Most AR problems are back-end symptoms of front-end mistakes. Investing in thorough eligibility verification, accurate registration, and upfront patient cost estimates reduces errors that create downstream denials. Implement Denial Tracking by Root Cause Don’t just work denials — analyze them. Categorize every denial by root