Introduction
Every healthcare provider — from a solo family physician to a large hospital network — faces the same operational reality: delivering great care is only half the battle. Getting paid for that care is the other half. And that is precisely where revenue cycle management in medical billing becomes mission-critical.
Whether you run a small clinic, a specialty practice, or a multi-location healthcare organization, a poorly managed revenue cycle costs you thousands of dollars every month in denied claims, missed charges, and administrative inefficiency. On the other hand, a well-optimized revenue cycle management process ensures that every service you render translates into timely, accurate reimbursement.
This guide covers everything you need to know: what RCM in medical billing means, how the RCM cycle in medical billing works end to end, what revenue cycle management services include, and how to choose the right approach for your practice. By the end, you will have a clear roadmap to protect your revenue, reduce billing errors, and improve your practice’s financial health.
What Is Revenue Cycle Management in Medical Billing?
Revenue cycle management (RCM) is the financial process that healthcare organizations use to track patient care episodes — from the initial appointment scheduling all the way through to the final payment collection. In the context of medical billing, RCM refers specifically to the administrative and clinical functions that contribute to capturing, managing, and collecting patient service revenue.
Simply put, RCM in medical billing is the system that ensures you get paid correctly, completely, and on time for the healthcare services you provide.
The term “revenue cycle” describes the entire journey of a single healthcare transaction:
- A patient schedules an appointment.
- The provider delivers a service.
- That service is documented and coded.
- A claim is submitted to the insurance payer.
- The payer adjudicates the claim.
- Payment is collected — from the insurer, the patient, or both.
Any breakdown at any point in this journey results in delayed payments, underpayments, or outright claim denials. That is why managing this cycle with precision and expertise is not optional — it is essential for financial sustainability.
Why RCM Matters More Than Ever
Healthcare billing has grown exponentially complex over the past decade. The transition to ICD-10 coding, the rise of value-based care models, the increasing patient financial responsibility shift due to high-deductible health plans, and the constant evolution of payer policies have all raised the stakes.
According to industry data, physician practices lose an estimated 5–10% of net revenue due to billing inefficiencies. For a practice generating $2 million annually, that represents $100,000 to $200,000 in preventable revenue loss every year. Effective revenue cycle management is the solution.
The Complete RCM Cycle in Medical Billing — Step by Step
Understanding the RCM cycle in medical billing is the foundation of improving your revenue performance. The cycle consists of several interconnected stages, each building on the last. Let’s walk through each one.
Stage 1: Patient Pre-Registration and Scheduling
The revenue cycle begins before the patient ever walks through the door. During pre-registration, staff collect:
- Patient demographics (name, date of birth, address, contact information)
- Insurance information (payer name, member ID, group number)
- Referral or authorization details if required
- Reason for visit
Accurate pre-registration is critical. A simple typo in a patient’s name or insurance ID number can cause a claim to be rejected weeks later. Many practices use automated tools to verify information at this stage, saving significant rework downstream.
Stage 2: Insurance Eligibility and Benefits Verification
Before the patient is seen, your billing team must verify that their insurance is active and confirm what their plan covers. This includes:
- Confirming the policy is active on the date of service
- Understanding deductibles, co-pays, and co-insurance
- Identifying services that require prior authorization
- Confirming network status of the provider
Eligibility verification is one of the highest-impact steps in the rcm cycle in medical billing. Skipping or rushing it causes a cascade of billing problems, including claim denials for inactive coverage or missing authorizations.
Stage 3: Prior Authorization
Some procedures, medications, and diagnostic tests require advance approval from the insurance company before they are performed. Failing to obtain prior authorization — or not following up when one is pending — is a leading cause of claim denials.
Robust revenue cycle management workflows include automated prior authorization tracking and escalation protocols so that no authorization is missed or expired.
Stage 4: Patient Check-In and Copayment Collection
When the patient arrives, your front desk staff should:
- Confirm all demographic and insurance information
- Collect the copayment or any known patient-responsibility balances
- Obtain necessary consent forms and signatures
Collecting copayments at the point of service dramatically improves collection rates. The cost and effort of collecting patient balances post-visit are significantly higher — and many balances are never collected at all.
Stage 5: Medical Coding
Once the provider completes the encounter, clinical documentation is translated into standardized codes. Medical coding involves:
- ICD-10 codes — for diagnoses
- CPT codes — for procedures and services rendered
- HCPCS codes — for supplies, equipment, and certain services
Accurate coding is essential for clean claim submission. Under-coding leaves money on the table. Over-coding can trigger audits and compliance issues. Correct coding — based on complete and precise clinical documentation — is the target.
Skilled medical coders are in high demand precisely because this step requires both deep clinical knowledge and expertise in billing guidelines from CMS, AMA, and individual payers.
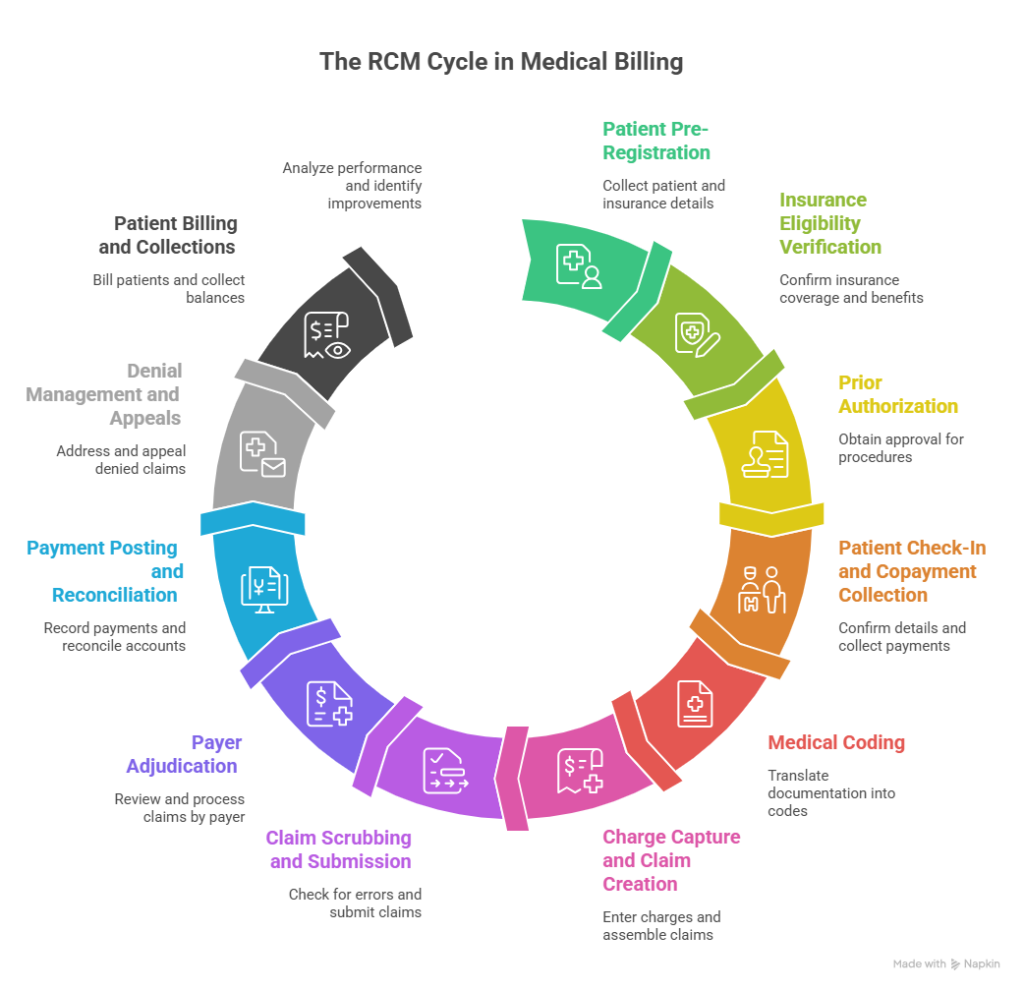
Stage 6: Charge Capture and Claim Creation
After coding, charges are entered into the billing system and a claim is assembled. The claim must include:
- Patient and provider information
- Diagnosis and procedure codes
- Date of service
- Place of service code
- National Provider Identifier (NPI)
- Payer-specific information
Charge capture audits help identify missed charges — services performed but never billed — which is a common but often overlooked source of revenue leakage.
Stage 7: Claim Scrubbing and Submission
Before a claim is sent to the payer, it goes through a “scrubbing” process. Claim scrubbing checks for:
- Coding errors (e.g., unbundling, incorrect modifiers)
- Missing or invalid data fields
- Payer-specific rule violations
- Duplicate claim flags
Clean claims — those that pass all edits — are submitted electronically to the appropriate payer. The goal is to achieve a clean claim rate above 95%, which means fewer denials and faster payment.
Stage 8: Payer Adjudication
Once the payer receives the claim, they review it against their coverage policies, fee schedules, and member benefits. The payer will:
- Approve and pay the claim (in full or partially)
- Deny the claim with a reason code
- Request additional information (e.g., medical records)
This process can take anywhere from a few days to several weeks, depending on the payer and the complexity of the claim.
Stage 9: Payment Posting and Reconciliation
When payment arrives — from the insurer as an Explanation of Benefits (EOB) or from the patient — it must be accurately posted to the correct patient account. Payment posting includes:
- Recording the payment amount
- Noting any contractual adjustments
- Identifying patient balances remaining
- Reconciling ERA (Electronic Remittance Advice) files
Accurate payment posting keeps accounts current and feeds into the denial analysis process.
Stage 10: Denial Management and Appeals
Denied claims are a reality in any medical billing operation. Effective RCM in medical billing requires a structured denial management process:
- Identify the denial reason code
- Determine if the denial is correctable and rebillable
- Correct and resubmit if appropriate
- File a formal appeal if the denial appears unjust
Practices that don’t actively work denials lose the associated revenue permanently. A denial management workflow that targets denials within 72 hours of receipt significantly improves collection rates.
Stage 11: Patient Billing and Collections
After insurance adjudication, any remaining balance becomes the patient’s responsibility. Clear, timely, and accurate patient statements improve collection rates and reduce confusion. Best practices include:
- Sending statements promptly after insurance payment
- Offering multiple payment options (online portal, phone, mail)
- Providing payment plan options for larger balances
- Using patient-friendly language in billing statements
Stage 12: Reporting and Analytics
The final stage of the RCM cycle in medical billing is analysis. Regular reporting on key performance indicators (KPIs) allows practices to identify bottlenecks, track trends, and continuously improve their revenue cycle performance. This stage closes the loop — insights gained feed back into improvements at every earlier stage.
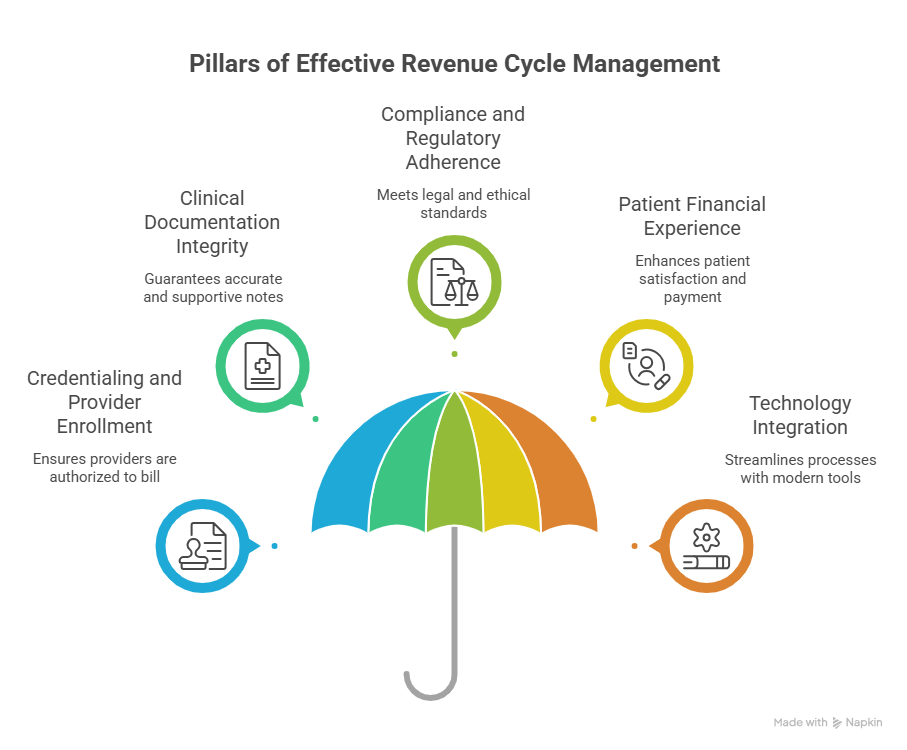
Key Components of Effective Revenue Cycle Management
Successful revenue cycle management rests on several foundational pillars:
1. Credentialing and Provider Enrollment
Providers must be enrolled with each payer network before claims can be submitted under their NPI. Credentialing delays can prevent a new provider from billing for months — a significant revenue impact for any practice.
2. Clinical Documentation Integrity (CDI)
Billing accuracy starts with documentation quality. If a provider’s clinical notes don’t clearly support the diagnosis and procedure codes submitted, claims will be denied and the practice may face compliance risk. CDI programs work with providers to improve documentation habits without disrupting clinical workflow.
3. Compliance and Regulatory Adherence
Healthcare billing is governed by a complex web of regulations — HIPAA, the False Claims Act, CMS guidelines, and state-specific payer rules. Non-compliance can lead to audits, penalties, and even exclusion from Medicare and Medicaid programs. A strong compliance program is a non-negotiable component of revenue cycle management.
4. Patient Financial Experience
As patient out-of-pocket costs rise, the patient financial experience has become a critical part of the revenue cycle. Practices that offer price transparency, financial counseling, and convenient payment options collect more patient balances and earn higher patient satisfaction scores simultaneously.
5. Technology Integration
Modern RCM relies heavily on technology — practice management systems (PMS), electronic health records (EHR), clearinghouses, and analytics platforms. Seamless integration between these systems reduces manual data entry, speeds up claim submission, and improves accuracy across the entire cycle.
Common Challenges in the RCM Cycle in Medical Billing
Even well-run practices encounter obstacles in the revenue cycle. Here are the most common pain points:
High Claim Denial Rates
Industry benchmarks suggest that the average denial rate for healthcare providers is 5–10%. However, some practices see denial rates as high as 20–30%. Common causes include:
- Eligibility issues (patient not covered on date of service)
- Missing or incorrect prior authorizations
- Coding errors (wrong modifiers, unbundled services)
- Duplicate claim submissions
- Late filing beyond the timely filing limit
Slow Accounts Receivable (A/R) Turnover
When claims sit unpaid for extended periods, cash flow suffers. Excessive A/R over 90 and 120 days is a red flag signaling that claims are being ignored rather than actively worked.
Front-End Errors
Up to 60% of claim denials originate from front-end errors — problems that occurred during scheduling, registration, or eligibility verification, long before a claim was ever submitted. Fixing revenue cycle problems must start at the front end.
Staff Turnover and Training Gaps
Medical billing is a specialized skill. High staff turnover — which is common in healthcare administration — leads to knowledge gaps, inconsistent processes, and revenue loss. Continuous training is essential.
Keeping Up with Payer Policy Changes
Payer billing guidelines change frequently and vary significantly from one insurer to another. Staying current requires dedicated resources and ongoing education.
What Are Revenue Cycle Management Services?
Revenue cycle management services refer to the professional services — provided by specialized companies or consultants — that help healthcare organizations manage some or all of the RCM functions described above.
RCM services can be comprehensive (full-cycle outsourcing) or targeted (addressing specific pain points such as coding, denial management, or credentialing).
What Do RCM Services Typically Include?
A full-service RCM provider typically offers:
- Patient eligibility verification — real-time insurance verification before every appointment
- Medical coding — certified coders for all specialties
- Charge capture — ensuring all services performed are billed
- Claim submission — electronic claims filed to all major payers
- Denial management — tracking, appealing, and resubmitting denied claims
- Payment posting — accurate reconciliation of all remittances
- Patient billing — patient statements and collections support
- Credentialing — provider enrollment with payer networks
- Reporting and analytics — dashboards and KPI reports to track performance
- Compliance support — audit preparation, coding audits, and policy compliance
Some RCM services providers also offer specialty-specific expertise — crucial for practices in areas like cardiology, orthopedics, behavioral health, or oncology where billing complexity is high.
Who Uses Revenue Cycle Management Services?
RCM services are used by a wide range of healthcare organizations:
- Independent physician practices
- Multi-specialty group practices
- Hospitals and health systems
- Ambulatory surgery centers (ASCs)
- Behavioral health practices
- Urgent care centers
- Dental and specialty practices
- Federally Qualified Health Centers (FQHCs)
The right revenue cycle management services partner understands your specialty’s billing nuances, your patient population’s payer mix, and the regulatory requirements in your state.
In-House vs. Outsourced RCM Services: Which Is Right for You?
One of the most common decisions healthcare practices face is whether to manage the revenue cycle internally or partner with an external RCM services provider. Here’s a side-by-side comparison.
In-House Revenue Cycle Management
Advantages:
- Direct control over billing staff and processes
- Immediate access to billing team for provider questions
- Potential cost savings for very large organizations with stable staff
Disadvantages:
- High overhead costs (salaries, benefits, training, software)
- Vulnerability to staff turnover and knowledge gaps
- Difficult to scale quickly with practice growth
- Harder to stay current with rapidly changing payer policies
Outsourced Revenue Cycle Management Services
Advantages:
- Access to specialized expertise across all payer types
- Lower overhead — no need to hire, train, or manage billing staff
- Technology included — no need to invest in separate billing software
- Scalable — services grow with your practice
- Better denial management through dedicated teams
- Performance-based accountability with clear metrics
Disadvantages:
- Less direct day-to-day control
- Requires clear communication channels and reporting agreements
- Not all providers are equally qualified — due diligence required
For most small to mid-sized practices, outsourcing revenue cycle management services delivers superior financial performance and a lower total cost than maintaining a full in-house billing department.
How Technology Is Transforming Revenue Cycle Management
Technology is reshaping every stage of revenue cycle management in medical billing. Here are the most significant technological advances transforming the field:
Artificial Intelligence and Machine Learning
AI-powered tools can now predict which claims are likely to be denied before they are submitted — allowing billers to fix errors proactively. Machine learning algorithms analyze patterns in denial data to surface systemic coding or documentation issues that human reviewers might miss.
Robotic Process Automation (RPA)
Repetitive, rule-based tasks — like eligibility verification, claim status checks, and payment posting — are ideal candidates for RPA. Automating these tasks reduces human error, speeds up processing time, and frees staff to focus on complex tasks that require judgment and expertise.
Patient Portals and Self-Service Payment
Digital patient portals allow patients to view their statements, understand their benefits, and make payments online — 24/7. Self-service options dramatically improve patient payment rates, as they remove friction from the collection process.
Cloud-Based Practice Management Systems
Cloud-based platforms give providers and billing staff real-time access to patient data, claim status, and financial reports from anywhere. Integration between EHR and billing systems eliminates duplicate data entry and reduces transcription errors.
Advanced Analytics and Business Intelligence
Modern RCM services leverage analytics platforms that go far beyond basic reporting. Predictive analytics can forecast A/R performance, flag high-risk claims, and identify trends in denial patterns — enabling data-driven decision-making that continuously improves financial performance.
Best Practices to Optimize Your RCM in Medical Billing
Regardless of whether you manage your revenue cycle in-house or with an outside partner, these best practices will help you optimize your RCM in medical billing:
1. Prioritize Front-End Accuracy
Invest in training and tools for patient registration, eligibility verification, and prior authorization. Preventing denials is far more efficient than appealing them after the fact.
2. Conduct Regular Coding Audits
Quarterly coding audits help identify patterns of under-coding, over-coding, or incorrect coding before they become systemic problems. Audits also support compliance and defend against payer audits.
3. Monitor Denial Trends
Track denial rates by payer, provider, denial reason code, and service type. Understanding why claims are denied allows you to make targeted corrections. A denial rate above 5% signals significant room for improvement.
4. Set and Track KPIs
Define clear performance benchmarks and track them consistently. Key metrics include:
- Days in A/R
- Clean claim rate
- First-pass acceptance rate
- Denial rate
- Net collection rate
- Cost to collect
5. Invest in Staff Training
Even the best billing system fails without knowledgeable staff. Regular training on coding updates (ICD-10, CPT annual changes), payer policy updates, and compliance keeps your team sharp and your claims clean.
6. Communicate with Providers About Documentation
Billing accuracy depends entirely on documentation quality. A feedback loop between billing staff and clinical providers — delivered diplomatically and with specific examples — improves documentation and coding accuracy over time.
7. Appeal Denials Systematically
Don’t let denials become write-offs by default. Build a structured appeal workflow with clear timelines, escalation paths, and tracking. Most denials are overturned on first appeal when properly documented.
8. Collect Patient Balances at the Point of Service
It is five times more expensive to collect a patient balance post-visit than at check-in. Train front desk staff to collect copayments and known patient responsibility amounts at every visit.
How to Choose the Right Revenue Cycle Management Services Provider
Selecting the right RCM services partner is one of the most consequential decisions your practice will make. Here is what to evaluate:
Specialty Expertise
Does the vendor have proven experience in your specialty? Billing for orthopedic surgery is very different from billing for behavioral health. Specialty expertise translates into fewer errors, faster claim resolution, and better reimbursement rates.
Technology Platform
What billing and analytics software does the vendor use? Can it integrate with your EHR? Ask for a demo and evaluate the reporting dashboard — you should have full visibility into your revenue cycle performance at all times.
Transparent Pricing
Most revenue cycle management services providers charge a percentage of collections — typically between 3% and 8%, depending on specialty and volume. Be wary of providers who are vague about fee structures or hide fees in the contract.
Performance Guarantees
Ask for industry-standard benchmarks and contractual commitments: a clean claim rate of 95%+, days in A/R under 40, and a denial rate below 5%. If a vendor is reluctant to commit to measurable outcomes, that’s a red flag.
Compliance Track Record
Verify that the vendor has a robust compliance program, including HIPAA-compliant data handling, regular coding audits, and documented compliance policies. Ask about any past OIG investigations or payer audits.
References and Case Studies
Request references from practices similar to yours in specialty, size, and payer mix. Case studies that demonstrate measurable improvement in collection rates or denial reduction give you concrete evidence of a vendor’s capabilities.
Communication and Reporting
How often will you receive performance reports? Who is your dedicated account manager? How quickly does the team respond to urgent issues? A strong RCM services partnership requires frequent, transparent communication.
Key Metrics Every Practice Should Track in RCM
Measuring the right KPIs is essential to managing and improving revenue cycle management. Here are the metrics every practice should monitor:
Days in Accounts Receivable (A/R)
This measures the average number of days it takes to collect payment after a service is rendered. Benchmark: Under 40 days. High days in A/R indicate slow claim processing, unresolved denials, or poor patient collections.
Clean Claim Rate
The percentage of claims that are accepted on first submission without errors. Benchmark: 95% or higher. A low clean claim rate signals upstream problems in registration, coding, or charge entry.
First-Pass Acceptance Rate
Similar to clean claim rate, this measures how many claims are paid on the first submission. A high first-pass rate means less rework and faster cash flow.
Denial Rate
The percentage of submitted claims that are denied by payers. Benchmark: Under 5%. Higher denial rates lead to delayed cash flow and increased administrative costs.
Net Collection Rate
The percentage of collectible revenue actually collected after contractual adjustments. Benchmark: 95–99%. This is one of the most important overall measures of revenue cycle efficiency.
Cost to Collect
Total cost of running the revenue cycle (staff, software, vendor fees) as a percentage of collections. Benchmark: 3–7%. Tracking this helps justify investments in technology or outsourced RCM services.
A/R Over 90 Days
The percentage of your total A/R that is more than 90 days old. Benchmark: Under 15–20%. High levels of aged A/R signal claims that are being ignored, disputed, or written off prematurely.
Patient Collection Rate
The percentage of patient-responsibility balances actually collected. As patient out-of-pocket costs rise, this metric deserves increasing attention.
Conclusion
Revenue cycle management in medical billing is the financial backbone of every healthcare practice. When it works well, cash flows predictably, denials are minimal, and your team can focus on patient care rather than chasing payments. When it breaks down, the consequences ripple across every part of your organization — from staff morale to patient satisfaction to the financial viability of your practice itself.
Understanding the RCM cycle in medical billing from end to end gives you the knowledge to identify where your revenue cycle is underperforming and what to do about it. Whether you choose to invest in stronger in-house processes, partner with experienced RCM services providers, or adopt new technology, the path forward starts with the same foundation: visibility, accuracy, and accountability at every step of the cycle.
If you’re ready to optimize your revenue cycle management, start with a comprehensive billing audit. Identify your current denial rate, clean claim rate, and days in A/R. Set clear benchmarks. Then build a plan — and a team — to close the gaps.
Your revenue cycle isn’t just a billing function. It’s the financial engine of your practice. Manage it with the same care and expertise you bring to your clinical care — and it will pay dividends for years to come.
