Introduction
Running a successful healthcare practice means more than delivering excellent patient care — it also means getting paid accurately and on time. Medical billing services have become essential for providers who want to reduce claim denials, speed up reimbursements, and eliminate the administrative burden that drains staff time and energy.
Whether you are a solo practitioner, a specialty clinic, or a multi-location healthcare group, understanding how professional medical billing works can transform your practice’s financial health. This complete guide walks you through everything you need to know — from the basics of medical billing to finding trusted medical billing services near me and implementing a robust revenue cycle management strategy.
What Are Medical Billing Services?
Medical billing services are specialized solutions that handle the process of submitting, tracking, and collecting payments for healthcare services rendered by providers. Instead of managing in-house billing staff, many practices outsource this function to dedicated billing companies or use advanced billing software platforms.
These services cover the full lifecycle of a claim — from patient registration and insurance verification to claim submission, denial management, and final payment posting.
Who Needs Medical Billing Services?
Medical billing solutions serve a wide range of healthcare providers, including:
- Primary care physicians and family practices
- Specialty clinics (cardiology, orthopedics, dermatology, etc.)
- Mental health and behavioral health providers
- Dental and vision practices
- Hospitals and outpatient facilities
- Urgent care centers and telehealth providers
Regardless of size or specialty, any provider that accepts insurance or processes patient payments can benefit from professional billing support.
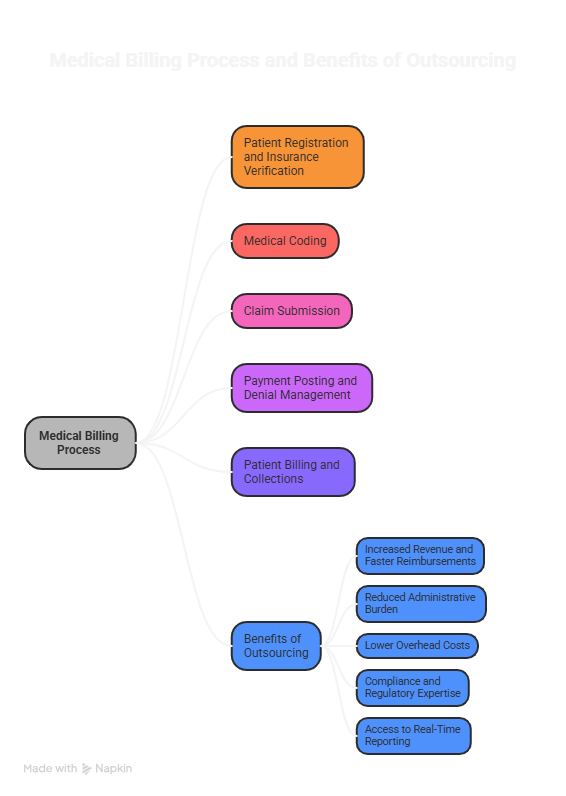
How Does the Medical Billing Process Work?
Understanding the step-by-step flow of medical billing helps providers appreciate the complexity involved and the value that expert billing teams bring to the table.
Step 1: Patient Registration and Insurance Verification
Before a patient is seen, billing teams verify insurance eligibility and coverage details. This prevents claim rejections caused by inactive policies or inaccurate demographic information.
Step 2: Medical Coding
Clinical documentation from the visit is translated into standardized codes — ICD-10 diagnosis codes and CPT procedure codes. Accurate coding is critical. Even minor coding errors can trigger denials or compliance audits.
Step 3: Claim Submission
Clean claims are submitted electronically to insurance payers. Timely submission is essential, as most payers enforce filing deadlines that, if missed, result in permanent non-payment.
Step 4: Payment Posting and Denial Management
Once payers process claims, payments are posted to patient accounts. When claims are denied, billing specialists review the reason, correct any errors, and resubmit. This appeals process is where expert billing teams truly demonstrate their value.
Step 5: Patient Billing and Collections
After insurance pays its portion, any remaining balance is billed to the patient. Professional billing services handle this diplomatically, protecting patient relationships while ensuring collections.
Key Benefits of Outsourcing Medical Billing Solutions
Outsourcing medical billing solutions offers measurable advantages over relying entirely on in-house staff. Here is why thousands of providers are making the switch.
1. Increased Revenue and Faster Reimbursements
Professional billing teams know how to submit cleaner claims the first time, reducing the denial rate significantly. Faster approvals mean money reaches your practice sooner — improving cash flow and financial stability.
2. Reduced Administrative Burden
Billing is time-consuming. When your front desk and clinical staff are focused on billing tasks, patient care suffers. Outsourcing frees your team to concentrate on what they do best — caring for patients.
3. Lower Overhead Costs
Hiring, training, and retaining in-house billing staff is expensive. Add the cost of billing software, compliance training, and employee benefits, and the numbers add up quickly. Medical billing services typically charge a percentage of collections — meaning you only pay when you get paid.
4. Compliance and Regulatory Expertise
Healthcare billing regulations change constantly. HIPAA requirements, payer-specific rules, and coding guideline updates demand ongoing education. Professional billing companies stay current so your practice remains compliant and audit-ready.
5. Access to Real-Time Reporting
Most modern medical billing services provide dashboards and reports that show your practice’s financial health at a glance — from days in accounts receivable to denial rates and collection performance.
Understanding Revenue Cycle Management in Medical Billing
Revenue cycle management in medical billing (RCM) refers to the end-to-end process of managing the financial interactions between a patient and a healthcare provider. It begins at the moment a patient schedules an appointment and ends when every dollar owed has been collected.
Medical revenue cycle management is broader than billing alone. It encompasses:
- Patient access management – scheduling, registration, prior authorizations
- Charge capture and coding accuracy
- Claim submission and payer follow-up
- Denial management and appeals
- Patient financial responsibility and collections
- Analytics and performance reporting
Why Revenue Cycle Management Matters
A fragmented revenue cycle is one of the top reasons healthcare practices lose money without realizing it. Studies consistently show that 5–10% of medical claims are denied on the first submission, and many of those denials are never reworked — leaving significant revenue uncollected.
Effective medical revenue cycle management closes those gaps. By identifying bottlenecks, correcting front-end errors, and aggressively managing denials, RCM specialists help practices recover revenue that would otherwise be written off.
In-House RCM vs. Outsourced RCM
| Factor | In-House RCM | Outsourced RCM |
| Cost | Fixed (salaries, training, software) | Variable (% of collections) |
| Expertise | Limited to staff knowledge | Dedicated specialists |
| Scalability | Difficult to scale quickly | Easily scalable |
| Technology | Requires investment | Included in service |
| Compliance updates | Staff must be retrained | Handled by provider |
For most small to mid-sized practices, outsourced medical revenue cycle management delivers a stronger return on investment.
How to Find Medical Billing Services Near Me
Searching for medical billing services near me can feel overwhelming given the number of providers in the market. Here is a practical framework to evaluate your options and choose the right partner.
1. Evaluate Their Specialty Experience
Not all billing companies handle all specialties equally. A billing firm experienced in mental health coding may not have deep expertise in surgical specialties. Always ask for references from providers in your specific specialty.
2. Check Their Technology Stack
Modern billing services should integrate seamlessly with your electronic health record (EHR) system. Ask about their practice management software, clearinghouse partnerships, and real-time reporting capabilities.
3. Review Their Track Record
Ask potential billing partners about their:
- First-pass claim acceptance rate (industry benchmark: 95%+)
- Average days in accounts receivable (target: under 35 days)
- Net collection rate (target: 95–99%)
4. Understand Their Pricing Model
Most billing companies charge between 4–9% of monthly collections, depending on specialty and volume. Be cautious of flat-fee models that do not incentivize strong collection performance.
5. Assess Communication and Transparency
Your billing partner should feel like an extension of your team. Look for companies that offer dedicated account managers, regular performance reviews, and prompt responses to your questions.
6. Verify HIPAA Compliance
Any billing company handling protected health information (PHI) must sign a Business Associate Agreement (BAA) and maintain rigorous data security standards. Never skip this step.
Types of Medical Billing Solutions Available Today
The medical billing landscape offers several models to fit different practice needs and budgets.
Full-Service Billing Companies
These firms manage your entire revenue cycle — from coding to collections. Best for practices that want a hands-off solution with full accountability.
Medical Billing Software Platforms
Cloud-based billing software gives practices more control while automating repetitive tasks like claim scrubbing and eligibility checks. Ideal for practices with experienced in-house billing staff who need better tools.
Hybrid Billing Models
Some practices use a combination — billing software for front-end tasks and an outsourced team for denial management and complex claims. This model balances control with expertise.
Specialty-Specific Billing Services
Certain companies focus exclusively on specific specialties such as behavioral health, radiology, or physical therapy. These niche providers often outperform generalist firms for complex coding scenarios.
Common Medical Billing Errors That Cost Providers Money
Even experienced billing teams can fall into patterns that erode revenue. Recognizing these common pitfalls helps you ask better questions when evaluating billing partners.
- Duplicate billing – Submitting the same claim twice leads to audits and penalties
- Upcoding or undercoding – Both carry compliance and financial risks
- Missing or incorrect modifiers – Modifiers communicate important context to payers; errors trigger denials
- Failure to obtain prior authorization – This is one of the most preventable denial causes
- Untimely filing – Missing payer deadlines results in permanent claim forfeiture
- Incorrect patient demographic information – A wrong insurance ID or date of birth can derail an otherwise perfect claim
A competent billing service will have quality assurance processes that catch these errors before claims go out the door.
Medical Billing for Specific Provider Types
Medical Billing for Physicians and Group Practices
Physician practices benefit most from billing services that specialize in Evaluation and Management (E/M) coding, procedure code bundling rules, and insurance contract analysis to ensure payers are reimbursing at contracted rates.
Medical Billing for Mental and Behavioral Health Providers
Mental health billing involves specific codes, session length documentation requirements, and payer-specific authorization processes. Specialized billing partners understand these nuances and can significantly improve collection rates for therapists, psychologists, and psychiatrists.
Medical Billing for Outpatient Facilities and Ambulatory Surgery Centers
Facility billing is distinct from professional billing and requires expertise in Ambulatory Payment Classifications (APCs), cost reporting, and Medicare’s Outpatient Prospective Payment System (OPPS).
Questions to Ask Before Hiring a Medical Billing Company
Before signing any contract, get clear answers to these critical questions:
- How long have you been providing medical billing services in my specialty?
- What is your first-pass claim approval rate?
- How do you handle denied claims, and what is your appeals success rate?
- What EHR and practice management systems do you integrate with?
- How will I receive financial reports, and how often?
- Who is my dedicated point of contact?
- What does your onboarding process look like, and how long does transition take?
- What are your contract terms, and is there an exit clause?
Getting written answers to these questions protects your practice and sets clear expectations from day one.
The Future of Medical Revenue Cycle Management
The healthcare billing landscape is evolving rapidly. Artificial intelligence and automation are reshaping how claims are scrubbed, denied claims are identified, and patient payment plans are offered.
Key trends transforming medical revenue cycle management include:
- AI-powered claim scrubbing that catches errors before submission
- Predictive analytics that forecast denial patterns by payer
- Patient payment portals and automated reminders that accelerate self-pay collections
- Real-time eligibility verification that eliminates front-end surprises
- Price transparency tools that help patients understand their financial responsibility upfront
Practices that partner with forward-thinking billing companies — those investing in technology and data-driven processes — will be better positioned to thrive as reimbursement models continue to evolve.
Conclusion
Medical billing services are no longer a luxury for large health systems — they are a practical necessity for any provider serious about protecting revenue and reducing administrative complexity. From accurate medical coding to aggressive denial management and transparent reporting, professional billing solutions give practices the financial backbone they need to grow sustainably.
Whether you are searching for medical billing services near me, exploring outsourced medical billing solutions, or looking to overhaul your medical revenue cycle management strategy, the right partner can make a measurable difference in your bottom line — and free you to focus on the patients who depend on you.
Ready to transform your practice’s financial performance? Start by evaluating two or three billing partners using the criteria in this guide, and take the first step toward a healthier revenue cycle today.
Frequently Asked Questions
What do medical billing services typically cost?
Most medical billing companies charge between 4–9% of monthly collections, depending on your specialty and claim volume. Some providers offer flat-fee models, though percentage-based pricing better aligns the billing company’s incentives with your practice’s performance.
What is the difference between medical billing and medical coding?
Medical coding is the process of translating clinical documentation into standardized alphanumeric codes. Medical billing uses those codes to create and submit claims to insurance payers. The two functions are closely related, and many billing services handle both.
Can small practices benefit from outsourced medical billing?
Absolutely. Small practices often benefit most from outsourcing because they lack the staff and resources to manage billing effectively in-house. Outsourcing levels the playing field, giving solo providers access to the same expertise and technology as larger health systems.
How long does it take to see results after switching billing companies?
Most practices see measurable improvement in claim acceptance rates and days in accounts receivable within 60–90 days of transitioning to a new billing partner. The onboarding and data migration process typically takes 2–4 weeks.
What is revenue cycle management in medical billing?
Revenue cycle management (RCM) in medical billing refers to the complete process of managing all financial interactions between a healthcare provider and patients or payers — from scheduling and insurance verification through claim submission, payment posting, and final collections.
How do I find medical billing services near me?
Start by searching online directories, asking for referrals from other providers in your specialty, and evaluating companies based on their specialty experience, technology, pricing, and track record. Local billing companies may offer more personalized service, while national firms often bring broader technology resources.
